Is there an effective treatment for Arthritis?

Is there an effective treatment for Arthritis? An overview for managing joint pain.
Are there any positives to having arthritis? Not really. It’s painful and it stops people doing the things that they love, or even just doing some of the most basic everyday tasks without significant pain.
What is arthritis?
Arthritis is an umbrella term which describes various musculoskeletal conditions that mostly involve joint pain and inflammation. Approximately 1 in 6 Australians have arthritis and it is the leading cause of chronic pain and disability after back pain. The most common form of degenerative arthritis (and the most common that we see in practice) is Osteoarthritis.
Osteoarthritis
Osteoarthritis, or OA for short, is a condition that involves degeneration of the joint and tends to be more common in those over the age of 40 years and/or with previous joint injuries. OA is often thought of as being ‘wear and tear’ on a joint, causing the joint to work extra hard to repair itself due to increased load. OA can be very painful, especially in the more advances stages. Some of the typical features include:
- Stiffness, decreased range of motion
- Inflammation, swelling, pain
- Joint cartilage damage
- Osteophytes – bone spurs growing around the joint
Approximately 1 in 11 Australian’s (2.2 million) have OA, with the most common joints including the spine, hands, hips, knees and ankles. It is a progressive condition and generally gets worse over time.

Joints typically wear out because load (activity) has continually exceeded the capacity that the joint can handle over time. This scenario is made many times worse if the range of motion at the joint is already poor, leading to improper loading of the joint surfaces. Add in some muscle weakness, instability and poor movement, then you’re on the fast-track to an arthritic joint.
What can we do about it?
There is no cure for Osteoarthritis. It is structural damage to the joint and once it is there we must shift our focus to slowing down the progression. While we can’t reverse the damage and restore healthy cartilage, we can control the rate of further degeneration and create an optimal environment around the joint.
Effective management should consist of:
- Load management; decreasing specific activities/load on the joint
- Maximising range of motion
- Increasing strength and stability
How do we do it?
We need to manage the load and identify the daily tasks, activities, hobbies, sports etc that have been causing increased joint loading. This can be a confronting situation for anyone faced with being told to stop doing what they love; sports, hobbies, etc. Reducing load on the joint is critical to decreasing inflammation and slowing down the degenerative processes while we continue to improve other factors that may allow some reintroduction of activity.
Once we have reduced load on the joint, we need to ensure that it has maximum range of motion. Beyond the damage to the joint itself, the primary reason for decreased range of motion is fibrosis of the soft tissues around the joint (muscles, tendons, ligaments, fascia). When our clinical testing shows decreased range of motion, we palpate the associated tissues for the presence of fibrotic adhesions that limit the motion. The OA itself is not reducible through manual treatment, but the fibrosis is! If it’s there (and it often is), we use highly specific hands-on techniques to break down the fibrotic adhesions and restore normal length to the soft tissues.
Once we’ve reduced fibrosis and achieved maximum range of motion, our focus shifts to getting the muscles stronger so that the joint is supported and able to better withstand load and activity. Targeted strength exercises are used to build up functional strength around the joint and this will often become part of an ongoing routine to maintain joint health.
Fibrosis is a big deal!
The importance of maximising range of motion can’t be understated! We often think of range of motion as being like blood pressure; just like if you had high blood pressure for long enough you are risking heart damage, having poor range of motion for long enough is increasing the likelihood of joint damage.
When soft tissues are infiltrated with fibrosis and become tight, short and inflexible, the range of motion changes and there is increased compression on the joint. Ideally we want full range of motion, with minimal compression, which ultimately preserves the cartilage and bone. When your movement is restricted by fibrotic tissues that can’t lengthen properly, the result is increased wear and tear at the joint surfaces, which is the fast-track to Osteoarthritis.
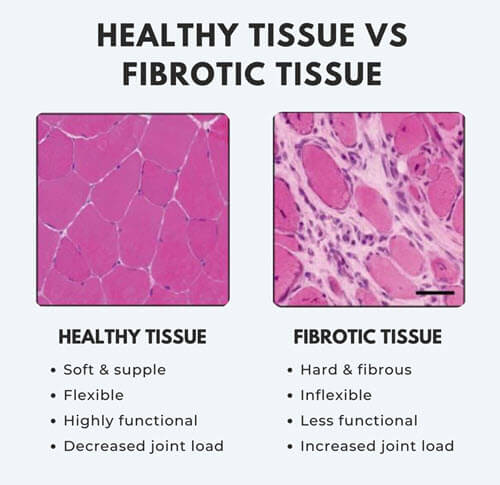
Research has also shown that strength in the muscles around an osteoarthritic joint is often dramatically decreased, as the presence of fibrosis is increased. The authors of the following 2018 paper suggested that the fibrosis may be a limitation on the regenerative potential of the muscles and excessive fibrosis can impair muscle strength. They proposed that the effectiveness of strength training for managing OA may have limited effect while the soft tissues are infiltrated by fibrosis.

Osteoarthritis is not reversible, but the soft tissue fibrosis is. By removing fibrotic adhesions we immediately decrease compressive load on the joint, improve range of motion and set the stage to increase strength and stability. In some cases, this may also substantially delay the need for a joint replacement.
Final thoughts
Arthritis, or more specifically Osteoarthritis, is a painful condition that we cannot totally cure, but we can slow it down and improve quality of life. Load management, range of motion and strength are the key features that must be emphasised to get the most out of degenerated joints and slow down the progression.
One of the major factors that can limit both range of motion and strength is fibrotic adhesions within the muscles, tendons and ligaments that support the joint. In our office we identify and reduce fibrosis to maximise range of motion and set the stage to get strong and stable. If you’ve been diagnosed with Osteoarthritis, but only been prescribed strength exercises without a detailed assessment of soft tissues, you may be leaving a lot on the table that can still be improved.
Dr. Christopher Aysom, Principal Clinician
BChiroSc, MChiro (Chiropractor)
Apex Soft Tissue & Spine
Pymble, NSW, Australia
https://apexsofttissue.com.au
Resources:
https://arthritisaustralia.com.au/types-of-arthritis/osteoarthritis/
https://www.aihw.gov.au/reports/chronic-musculoskeletal-conditions/osteoarthritis/contents/what-is-osteoarthritis
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7050996/


